Royal Raymond Rife
Symptoms
Psoriatic arthritis is a specific type of arthritis that occurs in
approximately 10 percent of the people who have psoriasis. It can start slowly,
with mild symptoms, or develop quickly. Generally, one or more of the following
symptoms may appear:
Discomfort, stiffness, pain, throbbing, swelling, or tenderness in one or more
joints and reduced range of joint motion;
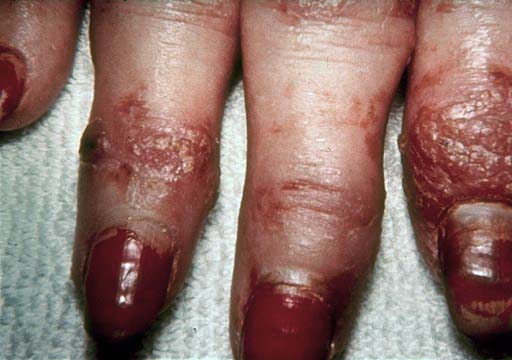
Affecting distal joints (the joint closest to the fingernail) in the fingers
or toes, lower back, wrists, knees, or ankles with swelling of the involved
fingers and toes suggesting a sausage appearance;
Morning stiffness and tiredness;
Nail changes may occur; e.g., the nail may separate from its nail bed and pits
may appear;
Inflammation of the eye, such as conjunctivitis.
Diagnosis
Psoriatic arthritis is similar to three other forms of arthritis which
may occur with psoriasis: rheumatoid, gout, and Reiter's syndrome. The diagnosis
of psoriatic arthritis is made on the basis of a medical history and physical
examination, blood studies, and x-rays of the joints that have symptoms.
A certain antibody generally present in rheumatoid arthritis is not usually
found in the blood of psoriatic arthritis patients. A blood test for the
antibody will distinguish between rheumatoid arthritis and psoriatic arthritis.
Fluid drawn from the affected joints can be examined to resolve the diagnosis
of gout or psoriatic arthritis.
Age of Onset / Developmental Factors
Psoriatic arthritis may develop at any age, but most often it begins
between the ages of 30 and 50. A number of factors seem to be associated
with the development of arthritis. Heredity has been shown to be a significant
factor. Recent studies have shown certain genetic markers which occur more
often in people who develop psoriatic arthritis. Also, there is speculation
that the immune system may play a role. Certain bacteria have been identified
as possible triggering factors and trauma has also been observed to trigger
psoriatic arthritis.
Treatments
A warm, stable climate may have some influence on psoriatic arthritis
symptoms, but diet has not been found to be beneficial in altering its course.
Treatments for mild psoriatic arthritis may include nonsteroidal anti-inflammatory
medicines such as aspirin and ibuprofen. Heat, warm water soaks, exercise
programs, splints, and physical therapy can also be used.
When psoriatic arthritis is not relieved or is more severe, more potent medications
may be required, e.g., methotrexate, gold injections and capsules, sulfasalazine,
etretinate and even PUVA. Surgery may also be required in some cases.
The Five Types of Psoriatic Arthritis
Symmetric Arthritis
Symmetric arthritis is much like rheumatoid arthritis. It usually
affects multiple pairs of joints and can be disabling. The associated psoriasis
is often severe. About 50 percent of people with this form of psoriatic arthritis
will develop variable degrees of progressive, destructive disease, although
it is less severe than rheumatoid arthritis.
Asymmetric Arthritis
Asymmetric (not occurring in the same joints on both sides of the
body) arthritis usually involves only one to three joints. It can affect
any joint, such as the knee, hip ankle and wrist. One finger can be involved
or many can be affected. The joints may be warm, tender and red. Individuals
may experience periodic joint pain which is usually responsive to medical
therapy.
Distal Interphalangeal Predominant (DIP)
This form of arthritis occurs in about five percent of people with
psoriatic arthritis. It involves primarily the distal joints of the fingers
and toes (the joint closest to the nail), and sometimes is confused with
osteoarthritis, a chronic arthritis of non-inflammatory character.
Spondylitis
In about five percent of individuals, inflammation of the spinal column
is the predominant symptom. Inflammation and stiffness of the neck, lower
back, sacroiliac, or spinal vertebrae are common symptoms making motion difficult.
There may be peripheral disease in the hands, arms, hips, legs and feet.
Spondylitis can also attack connective tissue such as ligaments.
Arthritis Mutilans
This is a severe, deforming and destructive arthritis which affects less than five percent of people with psoriatic arthritis. It principally affects the small joints of the hands and feet, although there is frequently associated neck or lower back pain. This type can progress over months and years. Arthritic flares and remissions tend to coincide with skin flares and remissions.
FREQUENCIES FOR HELPING ????
NPF Booklet on Psoriatic Arthritis
For an more detailed information on psoriatic arthritis, contact the NPF and request a copy of the NPF booklet on psoriatic arthritis. All NPF members are entitled to copies of NPF Booklets on a variety of topics.
Symmetric Psoriatic Arthritis
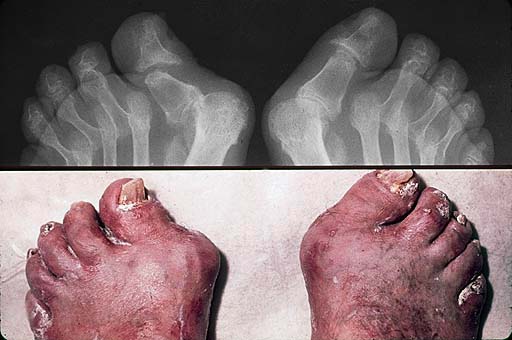
Symmetric Psoriatic Arthritis